The Raving Threat Of Monkeypox
Bayelsa State government on October 4, 2017 officially announced the outbreak of suspected deadly viral ‘Monkeypox’ epidemic in the state. The development shook the state to its foundations.
The disease struck a medical doctor and an 11-year-old boy. Eight other persons also came down with the disease. They were quarantined in an isolation centre at the Niger Delta University Teaching Hospital, Okolobiri. The centre was jointly set up by the state’s Ministry of Health epidemiological team and the Nigerian Centre for Disease Control (NCDC).
Besides the index cases, about 49 other persons who were suspected to have come in contact with persons infected by the monkeypox virus were placed under surveillance by the NCDC and the epidemiological team.
Like the Ebola virus disease outbreak in the country in 2014, the news of monkeypox epidemic spread like the wild harmattan fire within Bayelsa, causing panic among residents. Pronto, sanitisers which had disappeared after the Ebola epidemic was effectively tackled by the Federal Government, resurfaced again. As expected, residents started restricting themselves, avoiding handshakes and hugging. Sellers of bush meat and poultry business also began to experience low patronage in Yenagoa and its environs.
Professor Ebitimitula Etebu, the Commissioner for Health, who broke the news of the monkeypox outbreak in the state, said that samples of the virus had been sent to the World Health Organisation (WHO) laboratory in Dakar, Senegal, for confirmation.
He described the suspected monkeypox as a viral illness caused by a group of viruses that include chicken pox and smallpox. According to him, the first case was noticed in the Democratic Republic of Congo and subsequent outbreaks in the West African region.
Etebu explained that the virus has the Central African and the West African types, saying that the West African type is milder and has no records of mortality.
“Recently in Bayelsa State, we noticed a suspected outbreak of monkeypox. It has not been confirmed. We have sent samples to the World Health Organisation reference laboratory in Dakar, Senegal.
“When that comes out, we will be sure that it is confirmed. But from all indications, it points towards it. As the name implies, the virus was first seen in monkey, but can also be found in all bush animals such as rats, squirrels and antelopes.
“The source is usually all animals. It was first seen in monkeys and that is why it is called monkeypox. But every bush animals such as rats, squirrels, antelopes are involved. So, the secretions from particularly dead animals are highly contagious”, he stated.
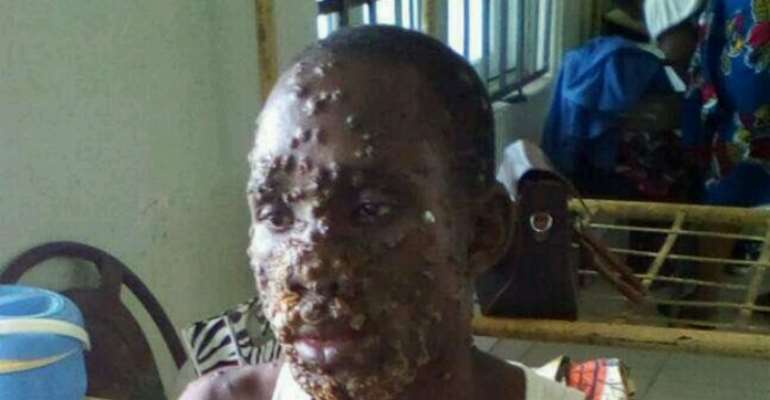
Etebu listed the symptoms of monkeypox as severe headache, fever, back pains amongst other symptoms, noting that most worrisome of all the signs were rashes bigger than those caused by chicken pox. He said the rashes are usually frightening and usually spread to the whole body of an infected person.
“We noticed the first index case (in Bayelsa) from Agbura where somebody was purported to have killed and eaten a monkey and after that the people who are neighbours and families started developing the rashes.
“We have seen cases from as far as Biseni. We invited the NCDC together with our own epidemiological team from the Bayelsa Ministry of Health. We have been able to trace most of the people who have come in contact with the patients.
“So far, we have 10 patients and we have created an isolation centre at the NDUTH and most of them are on admission and we are following up the 49 cases that we are suspecting might come down with the illness. As a state, we are taking care of all the expenses of all the isolated cases.
“The disease has an incubation period and it is also self-limiting in the sense that within two to four weeks, you get healed and it confers you with immunity for life.
“We have mobilised virtually every arsenal at our disposal in terms of sensitising the general public and making them aware by radio programmes, jingles, and fliers. So the Nigerian Centre for Disease Control has mobilised fully to Bayelsa State. We are on top the situation”, Etebu stated.
Both Agbura and Biseni communities are in Yenagoa Local Government Area of the state. However, an investigation showed that the 11-year-old boy from Agbura came down with the disease after having constant contact with a monkey, which he played with as a pet, contrary to speculations that he consumed monkey meat.
Some residents of Agbura who spoke on the disease said that only the 11-year-old boy and his six-year-old younger brother came down with symptoms of the epidemic and that the case of the younger brother was not as severe as his elder brothers.
“The victims used to play with the monkey. The monkey was like their pet. The monkey used to lick their bodies and climbed on them. That was all we know before their sickness occurred”, a resident who identified himself simply as Geoffrey, said.
While Bayelsa was battling to contain the monkeypox epidemic, the Federal Government, through the office of the Minister of Health, Professor Isaac Adewole, clarified that “the disease neither had a cure nor a vaccine”.
Two days after the official announcement of the epidemic outbreak, precisely on Friday, October 6, 2017, the number of infected persons in Bayelsa increased from 10 to 13 while persons who came in contact with victims also increased from 49 to 60.
Etebu, who gave an update on the epidemic, said the 60 cases “were being actively followed up at different located places in the state” for quick detection of new cases following exposure to suspected cases. He also gave out dedicated phone numbers for members of the public to call and report any suspected case in their neighborhoods.
While inaugurating a 12-member rapid response committee to monitor the spread of the disease, he expressed concern that “the situation could get out of hand if critical measures are not quickly put in place” because “new suspected cases are being detected everyday in the state”.
Etebu, however, allayed fears of the public and said that there was no need to panic as the state government was not leaving any stone unturned, adding that the government with the support of the WHO, international partners, and the NCDC, had embarked on enlightenment campaigns to sensitise the public on the monkeypox disease.
He said that active surveillance of the disease, case management, and other sundry measures had been carried out in a bid to halt the spread of the disease in the state.
“If you maintain simple hygiene of washing your hands when you touch animals, whether dead or alive, when you go to the toilet and such places, will help prevent the transmission of the disease”, the commissioner advised.
At the update event, Chief Medical Director of the NDUTH, Prof. Dimie Ogoina, stated that “none of the patients admitted in the hospital has died”, noting that the two index cases, the medical doctor and the 11-year-old boy, had fully recovered after treatment.
He said the NDUTH had been fully mobilised to receive and care for every suspected case of monkeypox that occurs in the state, adding that the tertiary health facility receives both children and adults suspected to have contacted monkeypox.
“We have created sufficient awareness among members of staff of the hospital. We need to protect health workers from the disease.
“We are training the health workers to have requisite skills and be able to care for patients and protect themselves. We are also training them on the use of personal protective equipment”, Ogoina said.
The Commissioner for Information and Orientation, Mr. Daniel Iworiso-Markson, announced a few days later that five more victims of the monkeypox illness had been discharged from the NDUTH, bringing the total number of those who had been treated and recovered from the disease to seven while those under supervision were responding positively to treatment.
Monkeypox facts
1. Monkeypox is a viral disease that produces pox lesions on the skin and is closely related to smallpox but is not nearly as deadly as smallpox was.
2. The history of monkeypox is new (1958), and the first human cases were diagnosed and differentiated from smallpox in the early 1970s.
3. Monkeypox virus causes monkeypox. The majority of cases are transmitted from animals (rodents) to humans by direct contact. Person-to-person transfer, probably by droplets, can occur infrequently.
4. Risk factors for monkeypox include close association with African animals (usually rodents) that have the disease or caring for a patient who has monkeypox.
5. During the first few days, symptoms are nonspecific and include fever, nausea, and malaise. After about four to seven days, lesions (pustules, papules) develop on the face and trunk that ulcerate, crust over, and begin to clear up after about 14-21 days, and lymph nodes enlarge. There may be some scarring.
6. The diagnosis of monkeypox is often made presumptively in Africa by the patient’s history and the exam that shows the pox lesions, however, a definitive diagnosis is made by PCR, ELISA, or Western blotting tests that are usually done by the CDC or some state labs. Definitive diagnosis is important to rule out other possible infectious agents like smallpox.
7. Treatment may consist of immediate vaccination with smallpox vaccine because monkeypox is so closely related to smallpox. Treatment with an antiviral drug or human immune globulin has been done.
